Corneal Ulcer – How to protect your Eye? 4 Home care treatment
Corneal Ulcer – How to protect your Eye? 4 Home care treatment
By Lowell
July 21, 2022
Health
 What is a Corneal ulcer?
What is a Corneal ulcer?
Overview
Corneal ulcers (also known as keratitis) are open sores on the cornea. In a similar way to how the crystal covers a watch face, the cornea covers the iris and the round pupil. Light enters the eye through the cornea, which is like a window. The cornea is protected by tears against bacteria, viruses, and fungus. Infections of the eye, severe dry eyes, or other eye disorders can result in corneal ulcers. Infections can result even from small injuries to the eye or from wearing contact lenses too long.
Symptoms
-
A red eye
-
There is severe pain and soreness in the eye
-
Other discharge or pus
-
Blurring of vision
-
Light sensitivity
-
Eyelid swelling
-
There is a white spot on your cornea that is either visible or not visible when you look in the mirror
In order to prevent blindness, corneal ulcers should be treated immediately as soon as they manifest symptoms. A corneal ulcer appears as a gray or white spot or area on the usually transparent cornea. Symptoms of corneal ulcers may not be visible without magnification, but you will feel them. Consult your ophthalmologist right away if you have any eye symptoms you are concerned about. You can lose your vision permanently if you do not treat corneal ulcers.
Causes
Many causes of corneal ulcers can be prevented. If you face the risk of injury to your eyes while working or playing, wear appropriate protective eyewear. Furthermore, if you wear contact lenses it is extremely important to properly care for them.
Infections leading to corneal ulcers include:
-
Acanthamoeba keratitis (Parasitic infections) – These are the most common amoebae in freshwater and soil. If Acanthamoeba enters the eye, it can cause a bad infection. This is particularly true for people who wear contact lenses.
-
Herpes simplex keratitis (Viral infections) – The condition is caused by stress, an immature immune system, or sun exposure. As well, the virus that causes chickenpox and shingles (the varicella virus) can trigger corneal ulcers.
-
Fungal keratitis (Fungal infections) – This condition is caused by improperly using contact lenses or eye drops that contain steroids, which lead to fungal infections that lead to corneal ulcers.
-
Bacterial infections – This occurs often in people who wear contact lenses, especially extended-wearing contact lens wearers.
Risk Factor

A corneal ulcer can occur in the following people:
-
Those who wear contacts
-
Those who have or have had cold sores or chickenpox
-
Steroid eye drops users
-
People who suffer from dry eyes
-
A person with an eyelid disorder that prevents the eyelid from functioning normally
-
Those who burn or injure their corneas
You can reduce your risk of corneal ulcers by handling, storing, and cleaning your contact lenses properly. Contact lenses need to be taken care of properly. You may find bacteria trapped under the lens from your lens cleaning solution or on the lens itself. Long-term lens wear can also block oxygen to your cornea, increasing the risk of infection. You might get a bacterial infection on your cornea after scratches on the edge of your contact. Also, a small amount of dust trapped under your contact lens could scratch your cornea.
How is a corneal ulcer diagnosed?
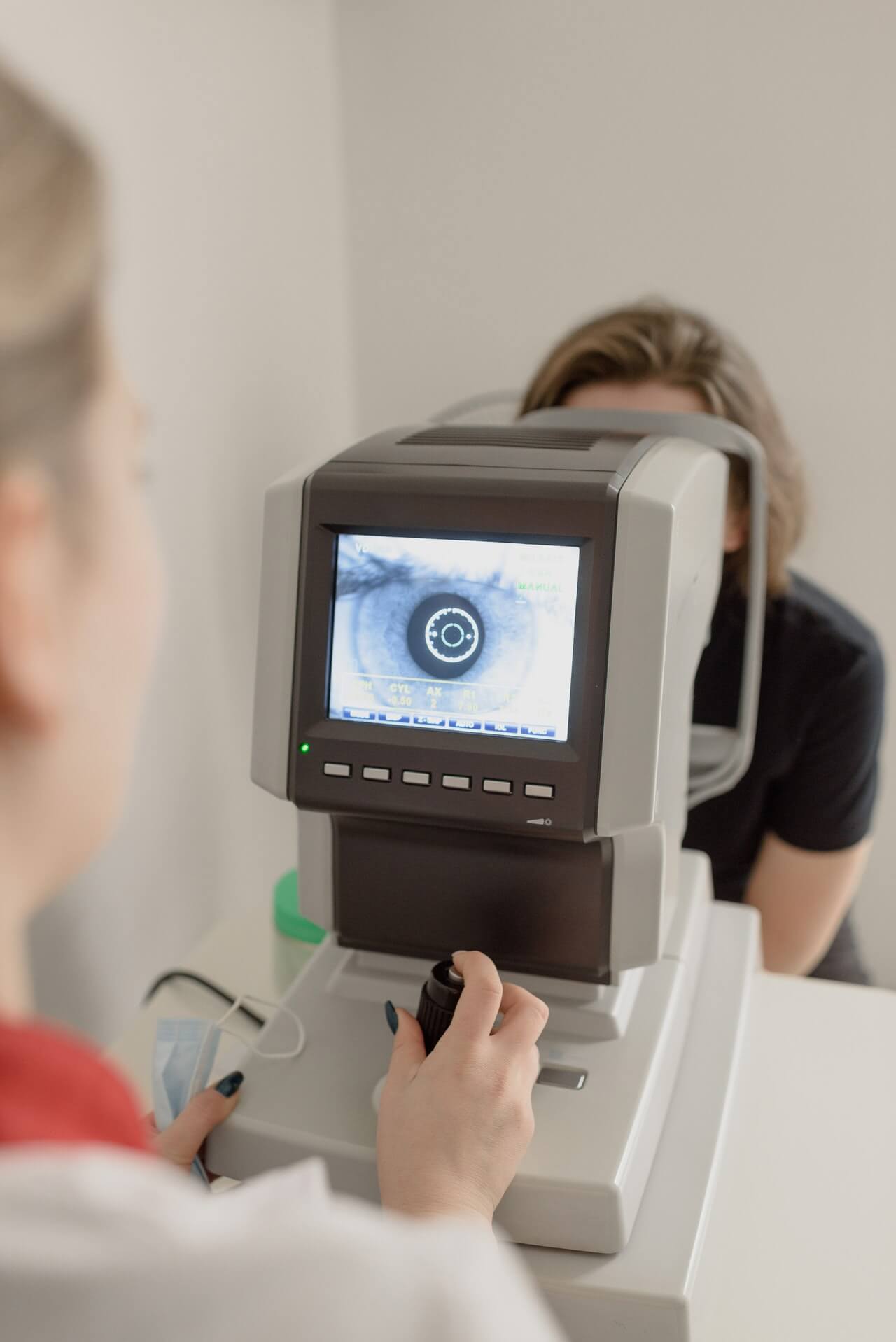
A corneal ulcer can be diagnosed during an eye exam by an eye doctor. An examination of your cornea will be performed using a special microscope known as a slit lamp. A slit lamp examination allows your ophthalmologist to check for corneal ulcers and see how much damage there is to the cornea. When the violet light strikes corneal damage, it will appear green. Your eye doctor will investigate an ulcer on your cornea to determine its cause. This is accomplished by using eye drops to numb the area around the ulcer, then gently scraping it to obtain a sample for testing. You can find out whether an ulcer contains bacteria, fungi, or viruses by performing a test.
How is Corneal Ulcer treated?
Based on the cause of your ulcer, you will receive the appropriate treatment. Among these are:
-
Medication. You may be prescribed antibiotics, antifungals, and antiviral eye drops. Your ophthalmologist may prescribe antifungal tablets. In other cases, the doctor may inject medication into your eye.
-
Surgery. A corneal transplant is sometimes necessary if the corneal ulcer is severe. You can restore your vision with a corneal transplant by replacing your damaged cornea with a healthy donor cornea. It is possible to leave a significant scar even when the infection has been treated with medication. A transplant may be performed in this case to improve vision.
4 Home Care Treatment
There are also some things you can do at home to ease symptoms, which your doctor may recommend:
1. Apply cool compresses to your eyes. However, make sure you keep water out of your eyes.
2. Touching or rubbing your eye with your fingers is not recommended.
3. Keep your hands clean and dry by washing frequently.
4. You may take acetaminophen or ibuprofen, which are over-the-counter pain medications.
Prevention
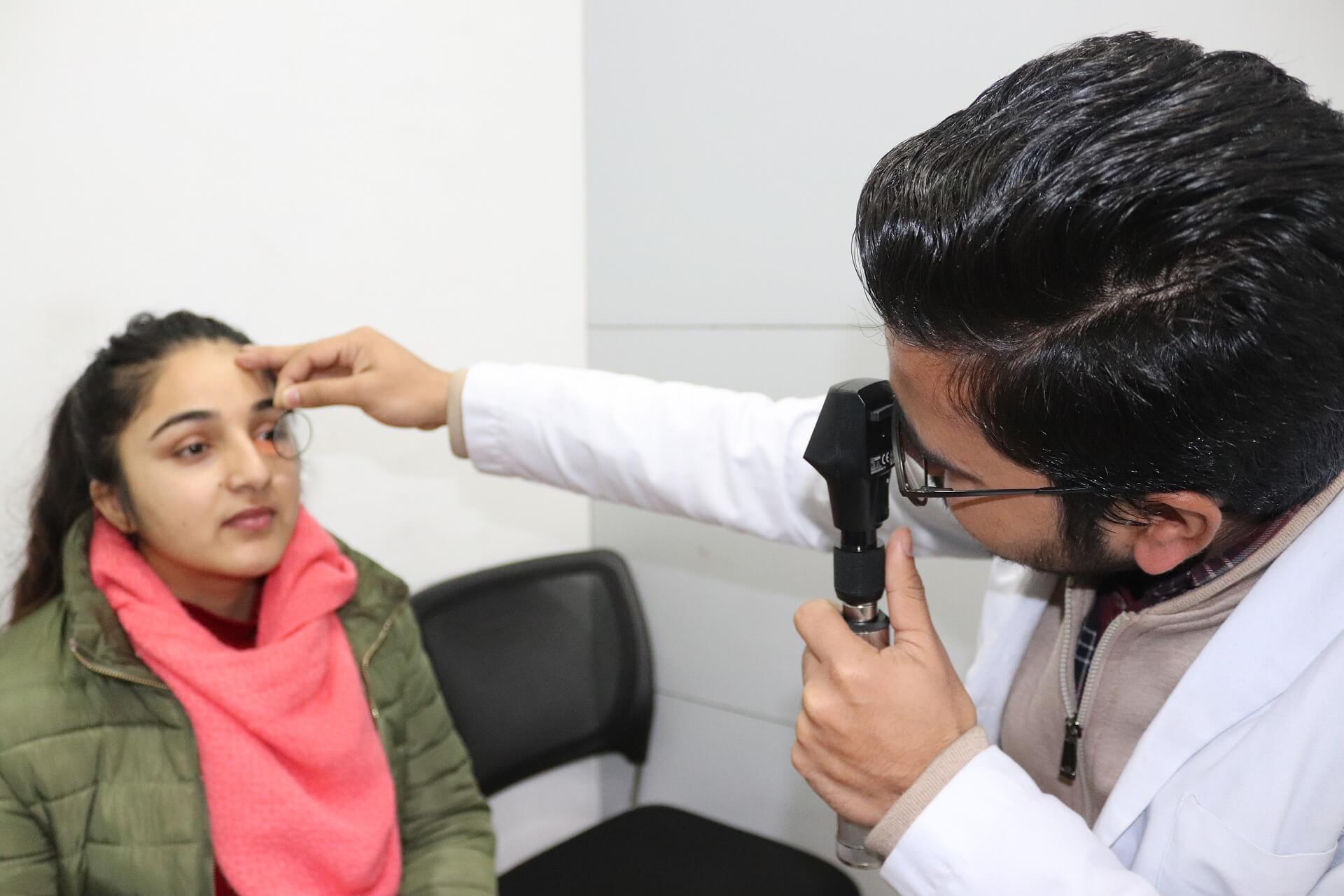
In case of any eye problems, you should see your doctor. An ulcer can develop from even the smallest injury. Avoid small particles by wearing protective eyewear.
When it comes to cleaning and wearing contacts, be very careful.
-
Before handling lenses, wash and dry your hands. Your mouth contains bacteria that can harm your cornea, so don’t use saliva to wet your lenses.
-
Contacts should never be worn while sleeping.
-
Lenses should be soaked in the disinfectant solution overnight.
-
When your eyes are irritated, remove your lenses. You shouldn’t put them back in until your eyes feel better.
-
Replace your contacts according to your doctor’s instructions.
Outlook
Medical emergencies. Occasionally, people can also develop serious loss of vision due to scarring over their retinas, in addition to visual obstruction. Scars on the eye can also result from corneal ulcers. It is rare for the entire eye to be damaged. Corneal ulcers can be treated, but sometimes they can cause a reduction in vision.
About Author

Lowell
 What is a Corneal ulcer?
What is a Corneal ulcer?